Permanent Impairment Assessment Explained
Navigating the aftermath of a serious accident involves more than just immediate medical care; it requires a deep understanding of the long-term consequences that an injury may have on an individual’s life. For both patients and legal professionals, the concept of permanent functional loss is a cornerstone of medical recovery and legal strategy.
The impairment assessment process refers to a lasting loss of physical or cognitive function that remains after a person has reached a specific medical plateau. Unlike temporary injuries that heal completely over time, these impairments are stable and unlikely to improve significantly despite further treatment. This distinction is crucial in the legal realm, as permanent impairment in personal injury cases often determines the level of compensation available for non-pecuniary damages, including pain and suffering, emotional distress, and loss of enjoyment of life.
Understanding Maximum Medical Improvement (MMI)
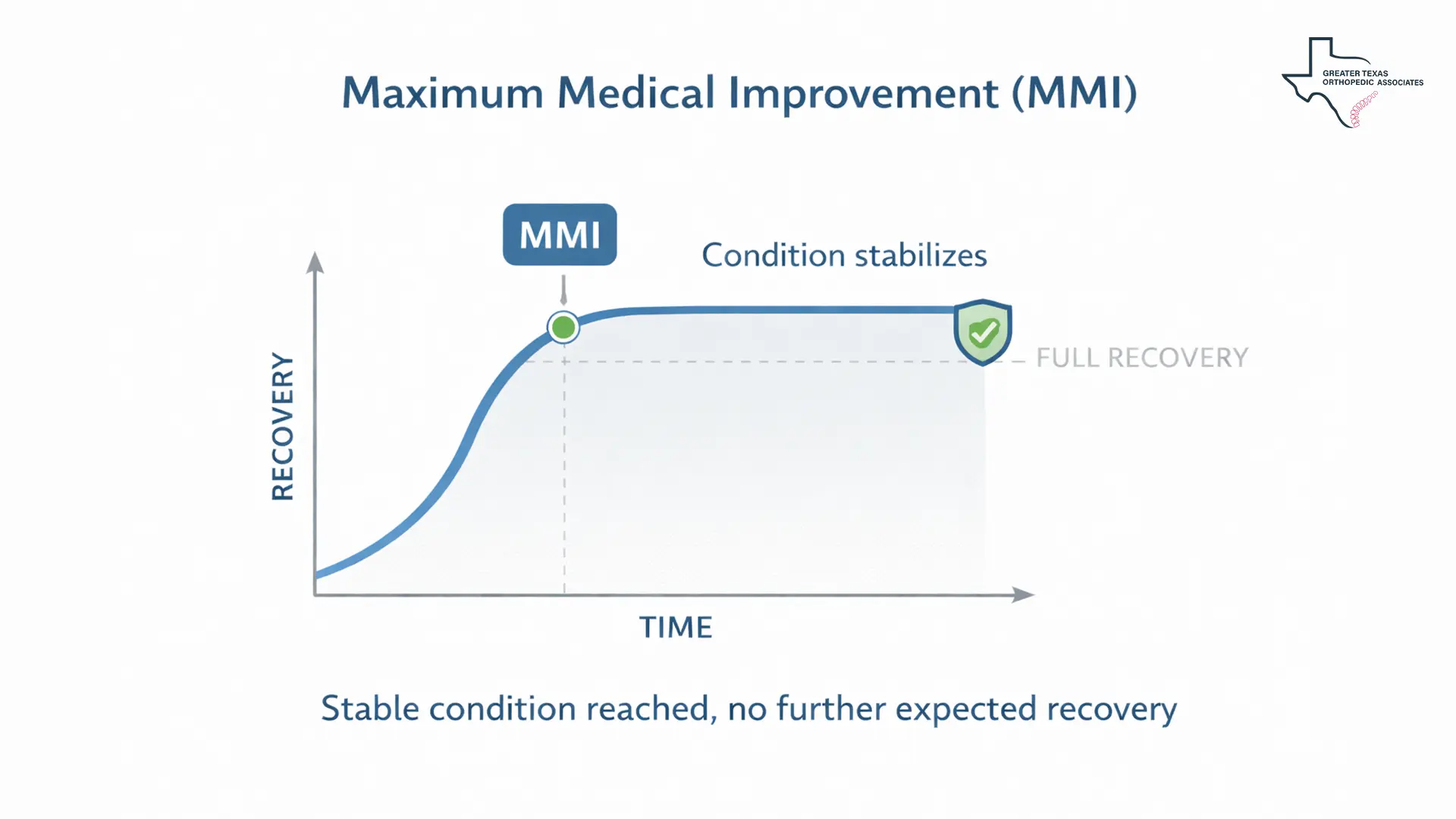
Before a specialist can perform a permanent impairment assessment, the patient must reach a milestone known as Maximum Medical Improvement (MMI). MMI is defined as the point in the recovery process where a patient’s condition has stabilized, and no further substantial improvement is expected from continued medical care. Reaching this stage does not necessarily mean the patient is pain-free or fully recovered. Instead, it signifies that the healing process has plateaued, and any remaining limitations are likely to be permanent.
For attorneys and insurance adjusters, MMI is a critical transition point. Before reaching this plateau, any assessment of long-term loss is considered premature and potentially inaccurate. Once a physician declares MMI, they can then begin the formal process of quantifying the residual functional loss. This process is how an impairment rating for injury claims is derived, providing a standardized numerical value to a patient’s permanent limitations.
Understanding the diagnostic steps leading to MMI helps explain why evaluations performed too early often fail to reflect the true extent of medically established impairment.
Impairment vs. Disability: A Key Distinction
It is important to clarify the difference between medical impairment and legal disability, as these terms are frequently used interchangeably in casual conversation but have distinct meanings in a professional context.
Impairment is a medical term describing the loss of use or a derangement of any body part, organ system, or organ function. It is a measurement of functional loss compared to a healthy, uninjured state. Disability, on the other hand, is a legal or socio-economic term. It refers to the effect that the medical impairment has on the individual’s ability to perform their job, participate in society, or complete activities of daily living.
While a physician provides a medical evaluation of impairment, the court or an insurance tribunal typically determines the degree of disability. For example, a minor loss of finger mobility might be a low medical impairment, but for a professional pianist, it could represent a total disability in their career. This is why how permanent impairment is evaluated must be precise and objective, focusing solely on the medical loss of function.
The Evaluation Framework: AMA Guides
The gold standard for performing a permanent impairment assessment is the American Medical Association (AMA) Guides to the Evaluation of Permanent Impairment. Used in over 40 states and multiple countries, these guides provide a reliable, repeatable, and transparent measurement framework. Adherence to these standards helps ensure that impairment reports remain consistent, transparent, and defensible across medical and legal settings.
The AMA Guides use a system to convert specific physical and psychological losses into a percentage of “Whole Person Impairment” (WPI). This standardized percentage reflects how much the permanent functional loss affects the entire body. For instance, a spinal injury might result in a 15% WPI rating, which serves as an objective piece of evidence in legal proceedings.
Depending on the jurisdiction, different editions of the AMA Guides may be used. Some states utilize the 4th, 5th, or the most recent 6th edition. Each version has its own methodology.
For example, the 6th edition prioritizes the Diagnosis-Related Estimate (DRE) method, while earlier editions often incorporate the Range of Motion (ROM) method. Knowing which standard applies to a specific case is essential for an accurate impairment rating for injury claims.
For a deeper discussion on the role of medical documentation in legal proceedings, see our related article on [Why Medical Documentation Matters in Injury Lawsuits.]
How Permanent Impairment is Evaluated
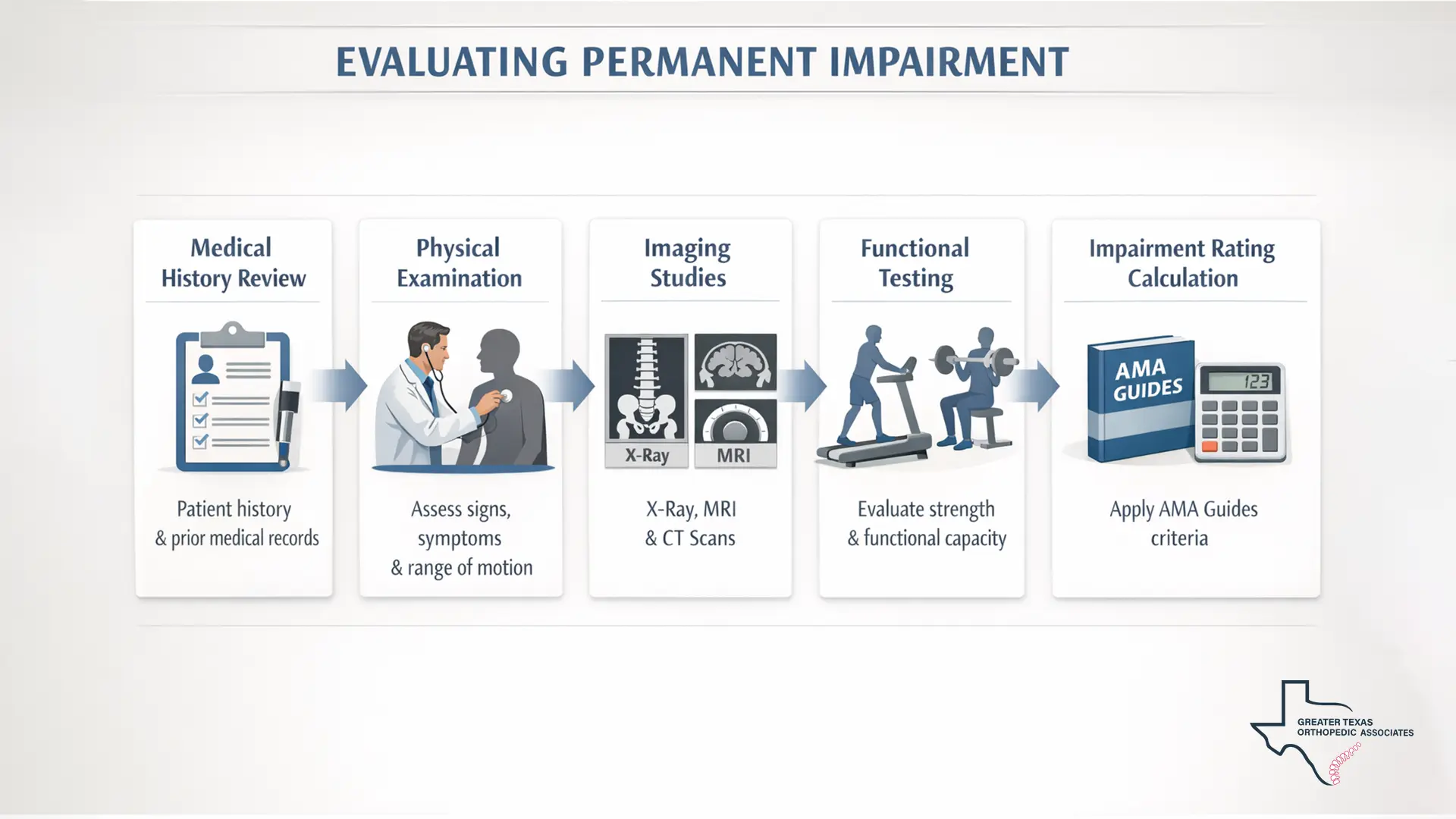
The process of determining a rating is structured and evidence-based. It begins with a comprehensive review of the patient’s medical history, starting from the initial trauma through the entire course of treatment. This ensures a clear connection, or “causation,” between the accident and the current functional state.
Following the history review, a specialized physician conducts a thorough clinical examination. During this exam, the specialist assesses the injury’s impact on the patient’s daily activities and work capacity. Objective diagnostic tools are heavily relied upon to support the findings. These tools include:
- Imaging: X-rays for bone structure, MRI for soft tissue and nerve damage, and CT scans for detailed anatomical views.
- Specialized Tests: Electromyography (EMG) and nerve conduction studies to assess nerve function.
- Functional Tests: Range-of-motion tests and muscle-strength assessments.
By combining these objective findings with the standardized tables in the AMA Guides, the specialist calculates the final rating. This systematic approach to how permanent impairment is evaluated ensures that the results are not merely subjective opinions but are substantiated by clinical data. Precision in this phase is vital, as incomplete documentation or a lack of objective findings can lead to a weakened legal claim.
The Role of Permanent Impairment in Personal Injury Cases
In personal injury litigation, demonstrating the permanency of an injury is often the factor that increases a case’s value. Insurance companies typically calculate settlement offers based on the severity and duration of the injury. Without a documented impairment, adjusters may attempt to settle a claim based only on past medical bills and short-term inconvenience.
When permanent impairment in personal injury cases is medically proven, the patient may be entitled to seek compensation for:
- Future Medical Expenses: Lifetime care, medications, or potential future surgeries.
- Loss of Earning Capacity: The impact on the patient’s ability to earn a living in the future.
- Non-Pecuniary Damages: Compensation for the lifelong human loss, including persistent pain and reduced quality of life.
For an attorney, a high-quality medicolegal report is a powerful tool for negotiation. It serves as neutral evidence that can help resolve disputes regarding the extent of an injury. If a case goes to trial, the impairment rating provides the jury with a clear, numerical measure of the accident’s impact.
Specialized Evaluations and Multidisciplinary Care
Complex injuries often require the expertise of multiple specialists. A traumatic brain injury (TBI), for instance, involves different evaluative criteria than a spinal fracture or a soft tissue tear.
In cases involving chronic back or neck pain, specialized interventional procedures can serve both a therapeutic and diagnostic purpose. For example, Medial Branch Blocks are used to confirm if the facet joints are the source of pain. If a patient experiences significant relief from these blocks, it validates the structural source of the impairment, which can then be documented in a permanent impairment assessment. Similarly, Epidural Steroid Injections help reduce nerve inflammation, allowing for a clearer assessment of the patient’s underlying functional capacity.
The Importance of Credible Documentation
The quality of the medical record is perhaps the most significant factor in the success of an impairment claim. Defense attorneys and insurance adjusters meticulously review every medical note to identify inconsistencies. If a patient initially reports back pain but later omits it, or if there are long gaps in treatment, the credibility of the impairment claim can be undermined.
To safeguard a claim, patients should:
- Seek immediate care: Initial evaluations should ideally occur within 72 hours of the injury to establish causation.
- Be consistent: Attend all follow-up appointments and physical therapy sessions.
- Report symptoms accurately: Do not downplay or exaggerate pain.
- Keep a journal: Documenting how the injury affects daily life can provide valuable context for the “non-economic” portions of a claim.
Faulty documentation, such as missing details or ambiguous language, often leads to confusion and weak evidence.
Reports prepared with medical-legal standards in mind are more likely to withstand forensic review and reduce disputes over credibility.
A more detailed discussion of common documentation errors can be found in our related article on [Common Medical Mistakes That Hurt PI Cases.]
The Path Toward Recovery and Resolution
A permanent impairment assessment is not simply a formality within a legal process; it is a critical step in defining the long-term reality of an injury. By objectively measuring permanent functional loss, this assessment helps clarify what aspects of a patient’s condition are unlikely to improve and what level of ongoing support may be required. In personal injury cases, this clarity reduces uncertainty and provides a stable foundation for both medical planning and legal decision-making.
When permanent impairment in personal injury cases is evaluated using standardized medical criteria, temporary symptoms can be clearly distinguished from lasting limitations. This distinction is essential for accurate treatment planning and for determining an appropriate impairment rating for injury claims. Whether the injury stems from a motor vehicle accident, a workplace incident, or a traumatic neurological condition, a structured medical evaluation ensures that conclusions are based on evidence rather than assumptions.
For patients, knowing that a permanent impairment assessment has been performed according to recognized medical guidelines can bring a sense of control and predictability, even when full recovery is not possible. For attorneys, objective impairment data allows for more precise case valuation and helps reduce disputes driven by speculation instead of clinical findings. In this way, a well-documented impairment assessment supports resolution by replacing uncertainty with medically grounded facts.
Conclusion
Understanding how permanent impairment is evaluated provides clarity at a point where uncertainty often dominates both medical recovery and legal decision-making. Reaching Maximum Medical Improvement, conducting a thorough clinical examination, and applying standardized frameworks such as the AMA Guides allow long-term functional loss to be defined with consistency and medical objectivity.
When permanent impairment is documented accurately, it becomes more than a clinical record. It serves as a reliable reference for treatment planning, case valuation, and long-term expectations. This structured approach helps distinguish lasting limitations from temporary symptoms and reduces disputes that often arise from incomplete or inconsistent medical evidence.
For both patients and attorneys, the strength of an injury claim rests on the quality of its medical foundation. A clear, evidence-based impairment evaluation supports informed decisions, fair outcomes, and realistic planning for the future. In complex personal injury cases, precision and consistency in medical documentation are not optional
they are essential.