Aggravation of a Pre-Existing Orthopedic Injury After a Car Accident
A pre-existing injury aggravated by car accident represents one of the most intellectually and clinically demanding challenges in modern orthopedics. In the aftermath of a collision, a patient often presents with a history of minor back pain, a previous joint surgery, or age-related degeneration. Insurance carriers frequently seize upon these histories, attempting to categorize the patient’s current suffering as a mere continuation of an inevitable biological process.
However, the human experience of trauma is rarely that linear. Most patients exist in a state of “compensated” health prior to an accident; they have underlying wear and tear, but they function without significant restriction. The accident acts as a catalyst, stripping away the body’s ability to cope. This measurable shift where manageable discomfort transitions into a disabling pathology is the pivot point of any personal injury claim with pre-existing condition.
Under the “Eggshell Plaintiff Rule,” Texas law recognizes that a negligent party is responsible for the damage they cause, even if the victim’s pre-existing fragility made the injury worse than it would have been for a healthy person. The burden, however, lies in the documentation. Proving aggravation requires moving beyond subjective reports of “feeling worse” and establishing objective clinical proof of a new, trauma-induced baseline.
What Is a Pre-Existing Injury Aggravated by Car Accident?
From a clinical standpoint, “aggravation” is a precise diagnosis. It is the demonstrable worsening of a pre-existing condition’s structural integrity or functional output due to external trauma. It is distinct from an “exacerbation,” which often implies a temporary flare-up of symptoms that eventually returns to the previous baseline.
For an orthopedic specialist to confirm an aggravation, they look for specific clinical markers:
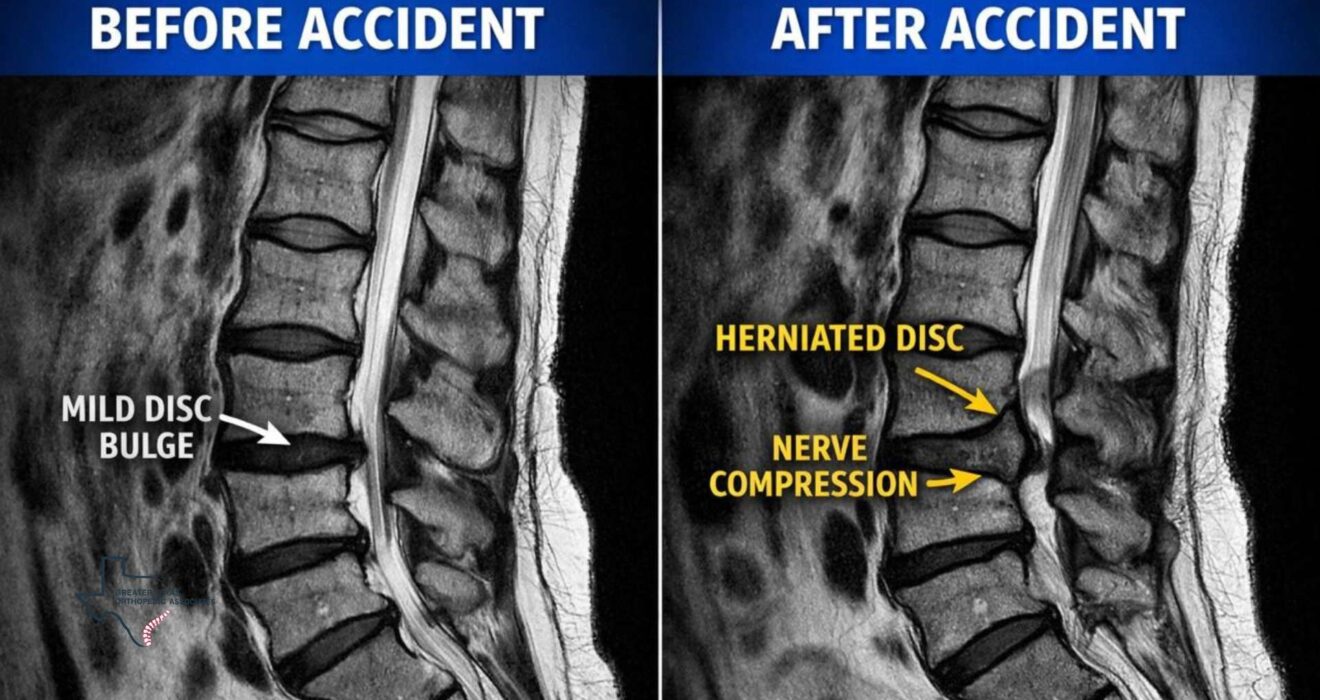
• Structural Progression: New findings on diagnostic imaging, such as an increase in the size of a disc herniation or the conversion of a partial-thickness tear into a full-thickness rupture.
• Neurological Decline: The emergence of new radiculopathy (pinched nerves), diminished reflexes, or muscle atrophy that was not present in prior records.
• Quantifiable Loss of Motion: A decrease in joint or spinal mobility measured in degrees using a goniometer.
Essentially, we are not looking for a “new” disease, but rather the acceleration of an old one. Many people live with “silent” findings on an MRI for years. Trauma can turn these previously silent findings into persistent symptoms that interfere with daily life and work activities.
Biomechanics of Trauma and Tissue Vulnerability
Understanding why an accident devastates a pre-existing injury requires looking at the physics of the human body under stress.
Acceleration and Deceleration Forces
During a collision, the body is subjected to massive kinetic energy. Even at moderate speeds, the rapid change in velocity (Delta-V) creates shear and compressive forces. Healthy tissue may tolerate these forces. Compromised tissue, however, often cannot.
Why Degenerated Tissue Fails
Degenerated tissues lack “structural reserve.”
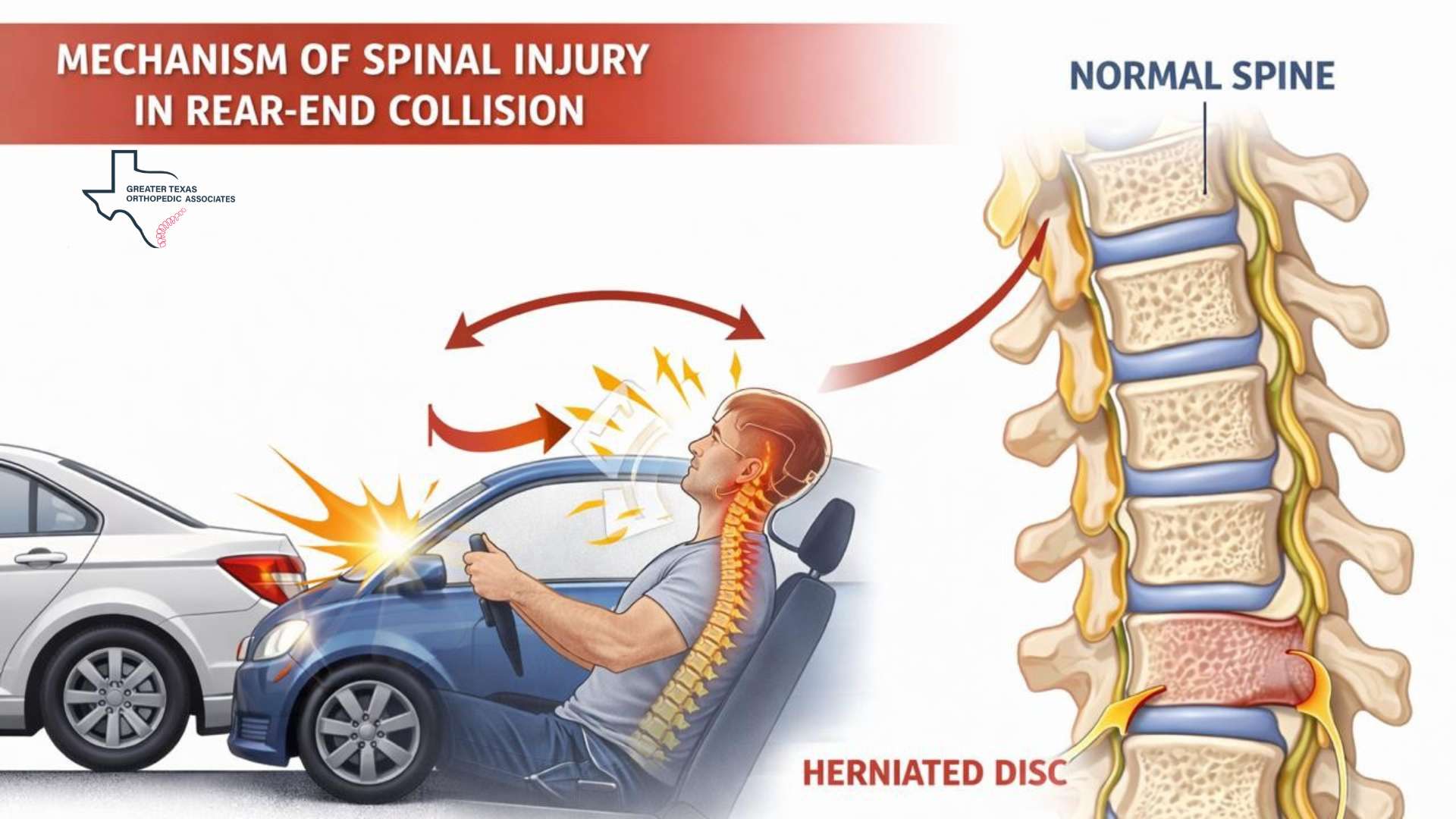
- The Spinal Disc: A healthy disc is a hydrated shock absorber. A pre-existing degenerated disc has lost height and elasticity. When a rear-end collision occurs, the “whiplash” motion, rapid extension followed by flexion, places extreme tension on the already brittle annular fibers of the disc.
- The Arthritic Joint: Arthritic cartilage is thin and pitted. When forced into a dashboard or jammed during bracing, the lack of a smooth gliding surface leads to “bone-on-bone” bruising (bone marrow edema), which can trigger a rapid downward spiral in joint health.
For a detailed explanation of lumbar disc injuries and how trauma affects spinal structures, see: 👉 Lumbar Disc Causes, Symptoms, & Treatment
Aggravation Versus Natural Degeneration
The “Natural Progression” defense is the primary tool used to deny claims. To counter this, an orthopedist must meticulously differentiate between the slow arc of aging and the sharp “step-down” of trauma.
The Timeline of Natural Progression
Aging is typically symmetrical and slow. Symptoms usually increase gradually over years, often correlating with age-appropriate wear seen on imaging. There is no single “event” that changes the patient’s life from Tuesday to Wednesday.
The Trauma Timeline
Traumatic aggravation is characterized by an acute onset. Patients describe a sudden loss of function; for example, they could walk a mile before the crash, but only a block afterward. Or they could lift 20 pounds before, but now struggle with a gallon of milk.
Orthopedic specialists evaluate two critical data sets:
- The Baseline (Pre-Accident): We review old pharmacy records, previous imaging, and employment history to see what the patient was actually capable of doing.
- The Shift (Post-Accident): We document the sudden need for more aggressive interventions, such as epidural steroid injections or surgical consultations, that were not on the horizon prior to the crash.
Objective Medical Documentation: The Only Defensive Proof
In a personal injury claim with pre-existing condition, the patient’s word is rarely enough. The legal system relies on objective findings that can be verified independently of the patient’s subjective complaints.
Comprehensive Clinical Exams
A complete examination in orthopedic clinics includes the following:
- Manual muscle testing: Graded on a scale of 0 to 5 to identify focal weakness.
- Skin mapping: Identify the exact location of sensory loss to correlate it with spinal levels.
- Gait analysis: See how the trauma has changed the patient’s basic mechanics.
Imaging: The “Before and After”
The gold standard of proof is comparative imaging. If we have an MRI from 12 months before the accident and another from one month after, we can pinpoint exactly what the trauma did. We look for “acute” signs, such as swelling in the bone (edema) or fresh tears in the ligaments, which prove the damage is recent.
For more information about impairment evaluation and how we quantify these losses, see:👉 Permanent Impairment Assessment
Legal Framework in Texas: The Reality of Liability
Texas follows the “Eggshell Plaintiff” doctrine, but it also operates under strict rules regarding “reasonable and necessary” medical expenses. Under Texas Civil Practice and Remedies Code Section 41.0105, a defendant is only liable for the additional harm they caused.
This means the legal battle often focuses on “apportionment.” In practical terms, medical reporting focuses on identifying how much the condition worsened after the crash compared to the patient’s prior functional level. The measurable increase in impairment following the crash is often the focal point of apportionment analysis.
Clinical Examples of Aggravation
The “Silent” Back Injury
A 50 year old with mild degenerative disc disease works a physical job without issues. After a rear-end collision, they develop “drop foot” an inability to lift the front of the foot. This is a clear, objective aggravation of a previously stable spinal level.
The Shoulder Bracing Injury
An elderly patient with known “mild” arthritis in the shoulder braces against the steering wheel during impact. The sudden force completes a partial rotator cuff tear that had been asymptomatic for years. The patient now requires surgery they would not have needed otherwise.
Temporary Flare-Up Versus Permanent Aggravation
Not every injury is permanent, and honesty in medical reporting is vital for credibility.
- Exacerbation/Flare-up: Increased pain and inflammation that settles back to the pre-crash baseline with 6-12 weeks of physical therapy.
- Permanent Aggravation: Structural changes (like a new herniation or bone fracture) that permanently alter the patient’s range of motion and pain levels.
Long-term follow-up is the only way to distinguish the two. If a patient is still unable to perform their job six months post-accident despite therapy, the aggravation is likely permanent.
The Critical Importance of Early Evaluation
In Texas personal injury claims, a documented gap in treatment can significantly weaken the credibility of a case. If a patient waits three weeks to see an orthopedist, the insurance company will argue that an “intervening event” like lifting a heavy box or sleeping wrong caused the new pain.
An early orthopedic assessment establishes the “Mechanism of Injury” (how the crash caused the specific physical damage) while the acute symptoms are still present. This creates a contemporaneous record that is much harder for insurance adjusters to dispute.
To understand what happens during a first orthopedic evaluation after injury, visit: 👉 Your First Orthopedic Evaluation After an Injury
Functional Limitations as Principal Evidence
Functional limitations provide a human context to medical data. We document specific losses:
- Occupational Impact: Can the patient still perform their “Essential Job Functions”?
- Activities of Daily Living (ADLs): Is the patient now dependent on others for dressing, driving, or household chores?
- Physical Endurance: Has their standing or sitting tolerance dropped significantly?
When these limitations are new, they serve as the most persuasive evidence that the accident caused a material change in the patient’s quality of life.
Conclusion
A preexisting injury aggravated by car accident is a medically definable reality. Having a prior condition does not automatically disqualify a claim, but it also does not automatically mean the case will succeed. In the end, the case stands or falls on the quality of the evaluation and the consistency of the medical record.
At Greater Texas Orthopedic Associates, we specialize in the meticulous analysis required to separate the “wear of time” from the “trauma of impact.” Without clear and objective medical evidence, it becomes extremely difficult to show how the patient’s condition truly changed after the accident.